It had been a long day: a book chapter due, tons of consults, too little sleep, procedures. So when I had a minute to grab a little respite from the chaos while nature called, I took it. I sat on the throne to ponder the day. I needn’t go into gory details. But when I stood up, I heard a “plunck.”
“What the…?”
And I turned around and saw it. My pager. In the toilet.
Now one must make some serious decisions quickly in this situation.
Like, “do I get it or flush it?” Hmmm.
Oh, hell, I’m a doctor. So I grabbed it quickly.
Then rinsed it. And I washed and washed my hands, mind you. No Purell for me! Nope, I don’t trust that crummy residue it leaves on your hands. Lots and lots of soap and water. Then chlorhexidine just to be careful.
But then I realized I had not checked the patient.
“Pager, pager are you alright?”
No response.
“Quick, call 911!”
Thinking quickly, I removed the battery cover and extracted the battery. I shook it dry. Still no response.
Then I couldn’t remember – is it 15 button pushes to two hard breaths or 5 button pushes to 1 hard breath? Feeling that hypoxia and drowning were the most likely cause of sudden death, I chose the latter. Do I push the buttons half an inch or a quarter of an inch? Oh hell, I don't know. How old was she? I should have probably used epinephrine, atropine, or isoproterenol, but felt this might be one patient where a “quick code” might be in everyone’s best interest. After all, I had had her for about 6 years, and someone had her before me. It was time.
So I called the code. Time of death: 07:12 AM.
But as an electrophysiologist, I decided that water might have induced electronic hypothermia, so I gave one more thing a try...
... I slowly rewarmed the patient by placing her above an incandescent bulb while saying her last rights. "Rest easy," I said and borrowed another pager.
Later that night, I returned to the patient to check on her. I replaced the battery, inspected for a pulse and “viola',” tones chirped from her underbelly! A successful resuscitation at last!
Damn.
-Wes
Thursday, November 30, 2006
Wednesday, November 29, 2006
The New Shareware?
Wow. Intel, Wal-Mart, and British Petroleum are joining hands (subscription required) in a "Kum Ba Ya" moment to try to develop an Electronic Medical Record (EMR) for their employees, housed on their own data warehouse creating the ultimate in shareware.
Hospitals, doctors, insurers, and the employers will have unfettered access to those records, but "they will belong to the employee." *Sigh*
But perhaps this data-sharing could be a good thing: fewer repeated tests, better continuity of care, a central repository of information where a consistent standard of information can be located. And yes, a wonderful place to see which doctors and hospitals are "performing" and which are not: who to pay, and who not to pay.
Employers are fed up with rising health costs and are rustling up their sleeves to do something about it. This, folks, is gonna happen.
The biggest issue now facing us: health care policy has to keep up with the advances in the EMRs being developed, or once your data is out there in the electronic ethos, it's out there for the millenium, just like, as the article says, "a Paris Hilton sex video."
-Wes
Hospitals, doctors, insurers, and the employers will have unfettered access to those records, but "they will belong to the employee." *Sigh*
But perhaps this data-sharing could be a good thing: fewer repeated tests, better continuity of care, a central repository of information where a consistent standard of information can be located. And yes, a wonderful place to see which doctors and hospitals are "performing" and which are not: who to pay, and who not to pay.
Employers are fed up with rising health costs and are rustling up their sleeves to do something about it. This, folks, is gonna happen.
The biggest issue now facing us: health care policy has to keep up with the advances in the EMRs being developed, or once your data is out there in the electronic ethos, it's out there for the millenium, just like, as the article says, "a Paris Hilton sex video."
-Wes
Tuesday, November 28, 2006
FDA and Pharma: Bed Partners?
After my Plaquequest post yesterday, I looked into the partnership arrangement between the FDA and BG Medicine a bit more today and found this statement from the FDA's own press release:
I wonder.
Sure makes those pens and lunches from drug reps seem like chump change, doesn't it?
Anybody else want to weigh in on this?
-Wes
The agency ... concluded an agreement with BG Medicine, a biotechnology research company, to collaborate on discovering signs of liver toxicity in the initial stages of drug development.BG Medicine's press release was a bit more detailed:
25 Oct 2005: BG Medicine, a Massachusetts-based biotechnology research company, today announced the submission of a Cooperative Research and Development Agreement (CRADA) with the Food and Drug Administration's National Center for Toxicological Research (NCTR), to jointly conduct a liver toxicity study designed to overcome one of the primary obstacles to the efficient development of safe and effective drugs. The study, Liver Toxicology Biomarker Study (LTBS), aims to discover biomarkers of human hepatotoxicity in the standard test used by pharmaceutical manufacturers in the initial stages of drug development.Now I'm not sure what I think about this. The FDA is supposed to assure the safety of pharmaceuticals to the public. While the bureaucratic quagmire called the FDA certainly needs to streamline their approval of drugs, are they able to maintain their objectivity regarding drug evaluations when they've become "best buddies" with the pharmaceutical industry by using Big Pharma's funds and facilities like this?
Liver toxicity is the most common biological reason for drug failure in the development of new pharmaceuticals, affecting one in six drugs in development. The toxicity tests currently in use by drug companies have been unchanged for at least 40 years and often fail to identify human liver toxicity issues. Consequently, liver toxicity is often detected for the first time when drugs are in phase 2 of clinical testing after tens of millions of dollars or more have been spent on a drug.
On March 16, 2004 the FDA released a report, "Innovation/Stagnation: Challenge and Opportunity on the Critical Path to New Medical Products," describing the "urgent need to modernize the medical product development process -- the Critical Path -- to make product development more predictable and less costly." The proposed project addresses the liver toxicity issue highlighted in the Critical Path document as one of the obvious and priority areas for innovation.
The CRADA process is a standard procedure for studies the FDA undertakes in collaboration with private companies. The liver toxicity study has been designed by BG Medicine and the FDA with input from a number of pharmaceutical companies. The study will be funded by and conducted in collaboration with pharmaceutical manufacturers. (Emphasis mine)
The research project leverages NCTR's and BGM's systems biology platforms for functional genomics, proteomics, metabolomics and computational analysis.
The LTBS will be conducted at the FDA's NCTR laboratory in Jefferson, Arkansas and at BG Medicine in Waltham, Massachusetts. The study is open to participation by all pharmaceutical manufacturers. Participating companies will receive a paid-up perpetual license to any biomarkers discovered and access to all project data.
I wonder.
Sure makes those pens and lunches from drug reps seem like chump change, doesn't it?
Anybody else want to weigh in on this?
-Wes
Played for Performance
Pay for Performance: To think our government, legislators, and insurance yahoos want to implement this for Medicare payments to physicians and hospitals. Look what it has come to in England.
Yuck.
-Wes
Yuck.
-Wes
Monday, November 27, 2006
Plaquequest
Today the hunt for the vulnerable plaque will begin in earnest. It's not a new adventure, but one I like to think of a "Plaquequest."
"Vulnerable plaque" is the plaque within an artery that can suddenly "rupture" and stimulate the rapid formation of clot within a coronary artery, compromising blood flow to a portion of heart muscle, and leading to a heart attack. Cardiologists have long recognized that tightly narrowed arteries are not necessarily the ones that suddenly occlude during a heart attack; sometimes only modestly narrowed arteries become abruptly occluded. This has lead to a search for ways to identify which plaques are vulnerable to rupture before rupture occurs, potentially saving lives and heart muscle.
A consortium of researchers are assembling to attempt to identify vulnerable plaque. To the tune of $30 million. It is a huge undertaking, but the pot of gold at the end of the rainbow is just too tempting for industry to ignore. It is not surprizing that Merck and Astra Zeneca, two large pharmaceutical companies have joined the hunt. But BG Medical? Who are they? Described as a new "start-up company" in the New York Times, it's really a consortium of pharmaceutical and imaging industry interests including Astra Zeneca, Boehringer Ingelheim, Biorosettex, GlaxoSmithKline, Philips, Mitsubishi Pharma Corporation, the "Global Alliance for TB Drug Development" (what has tuberculosis got to do with this? I wonder if their membership is happy about this investment, but I digress) and...
..the FDA.
Really? The Food and Drug Administration is now a "Partner" with BG Medical? Maybe so. At least they're listed on BG Medical's "Innovative Paths to a Trusted Partner" page on their website. Certainly, there have been concerns regarding conflicts of interest with the FDA's "Special Government Employees" that advise the FDA having conflicts of interests with the pharmaceutical industry and what needs to be disclosed to the public. But to this doctor, the FDA itself has a responsibility to the public at large to maintain objectivity in its oversight of new drugs during the approval process. Certainly this partnership of the FDA itself with BG Medical violates the public's trust.
Oh, but we needn't stop here.
Look who else is "partnering" in Plaquequest: Humana, a manager of health care insurance plans.
Plaquequest is a noble goal indeed. Going after arteries already blocked is a $6 billion stent market. $20 billion more are spent for statin drugs for primary and secondary prevention of coronary disease presently. It seems clear that the drug and device industry wants to know if they can boldly grow this market so cardiologists can place stents in asymptomatic arteries cloaked under the "vulnerability" guise. Interesting, but will this work?
Lets say this research succeeds at Plaquequest. How do we apply this finding to John Q. Public? Do we then place a stent there knowing it could thrombose as a result of the stent being there? Or should we place everyone on a statin drug as we've already been recommended for anyone with significant hyperlipidemia. Doctors haven't historically been so good at even this simple recommendation. And imaging to screen for vulnerable plaque is expensive: who is going to pay for massive screening tests? (Take a guess) So what have we gained?
It's hard to know. Maybe some new drugs or insights to the mechanism of acute coronary syndromes will be discovered, leading to new research paths for these great companies. But I hope Plaquequest is more than a means for Humana to get more best practice and cost analysis data while doctors get to feel good that the pharmaceutical and medical imaging industry has "given back" to research centers, and maybe the FDA.
-Wes
"Vulnerable plaque" is the plaque within an artery that can suddenly "rupture" and stimulate the rapid formation of clot within a coronary artery, compromising blood flow to a portion of heart muscle, and leading to a heart attack. Cardiologists have long recognized that tightly narrowed arteries are not necessarily the ones that suddenly occlude during a heart attack; sometimes only modestly narrowed arteries become abruptly occluded. This has lead to a search for ways to identify which plaques are vulnerable to rupture before rupture occurs, potentially saving lives and heart muscle.
A consortium of researchers are assembling to attempt to identify vulnerable plaque. To the tune of $30 million. It is a huge undertaking, but the pot of gold at the end of the rainbow is just too tempting for industry to ignore. It is not surprizing that Merck and Astra Zeneca, two large pharmaceutical companies have joined the hunt. But BG Medical? Who are they? Described as a new "start-up company" in the New York Times, it's really a consortium of pharmaceutical and imaging industry interests including Astra Zeneca, Boehringer Ingelheim, Biorosettex, GlaxoSmithKline, Philips, Mitsubishi Pharma Corporation, the "Global Alliance for TB Drug Development" (what has tuberculosis got to do with this? I wonder if their membership is happy about this investment, but I digress) and...
..the FDA.
Really? The Food and Drug Administration is now a "Partner" with BG Medical? Maybe so. At least they're listed on BG Medical's "Innovative Paths to a Trusted Partner" page on their website. Certainly, there have been concerns regarding conflicts of interest with the FDA's "Special Government Employees" that advise the FDA having conflicts of interests with the pharmaceutical industry and what needs to be disclosed to the public. But to this doctor, the FDA itself has a responsibility to the public at large to maintain objectivity in its oversight of new drugs during the approval process. Certainly this partnership of the FDA itself with BG Medical violates the public's trust.
Oh, but we needn't stop here.
Look who else is "partnering" in Plaquequest: Humana, a manager of health care insurance plans.
The centerpiece of the research will be a study of 4,000 to 6,000 Humana patients with at least two known risk factors for heart attacks. As the outcome for the patients becomes clear over the next few years, researchers hope the profiles that emerge from the study will, in hindsight, show patterns pointing directly to the high-risk patients who actually suffered heart attacks. That in turn could help the companies create new therapeutic products.I'm not sure of their motivation here, but I wonder how much revenue and "best practices data" they receive for supplying the patients for this trial. Hmmm. It seems only Humana patients will be participating in this "research." Why?
Plaquequest is a noble goal indeed. Going after arteries already blocked is a $6 billion stent market. $20 billion more are spent for statin drugs for primary and secondary prevention of coronary disease presently. It seems clear that the drug and device industry wants to know if they can boldly grow this market so cardiologists can place stents in asymptomatic arteries cloaked under the "vulnerability" guise. Interesting, but will this work?
Lets say this research succeeds at Plaquequest. How do we apply this finding to John Q. Public? Do we then place a stent there knowing it could thrombose as a result of the stent being there? Or should we place everyone on a statin drug as we've already been recommended for anyone with significant hyperlipidemia. Doctors haven't historically been so good at even this simple recommendation. And imaging to screen for vulnerable plaque is expensive: who is going to pay for massive screening tests? (Take a guess) So what have we gained?
It's hard to know. Maybe some new drugs or insights to the mechanism of acute coronary syndromes will be discovered, leading to new research paths for these great companies. But I hope Plaquequest is more than a means for Humana to get more best practice and cost analysis data while doctors get to feel good that the pharmaceutical and medical imaging industry has "given back" to research centers, and maybe the FDA.
-Wes
Sunday, November 26, 2006
Infectious Disease: Bad Place for Malpractice Law
It's amazing how fast plantiff's lawyers will dump their clients seeking compensation for acquiring MRSA infections in Kentucky once real data regarding infection rates (and the difficulties with their interpretation) become available.
-Wes
-Wes
Friday, November 24, 2006
James Bond: Saved by A Defibrillator

Tonight I learned that my field, cardiac electrophysiology, has finally reached prime time. If you haven’t had the chance, catch Casino Royale, one of the better James Bond flicks to hit the screen. Lots of action, a slightly more believable plot (can that happen?) and plenty of eye candy for all.
But best of all, I got to watch James (Daniel Craig) try to defibrillate himself! It happens after James Bond is poisoned by as tainted martini with “digoxin” at the poker table. He then develops blurred vision and moderate disorientation, and quickly excuses himself from the poker table. He then staggered to grab a shaker of salt and a glass, and proceeded to the bathroom, where he quickly induced vomiting. He then staggered to his Aston Martin Vanquish and opened the glove compartment…. and there it was: an automatic external defibrillator! Yep, smaller and more compact than commercially-available models, but a defibrillator nonetheless.
It turns out that a small chip implanted in James’ arm told his compatriots back at his headquarters that he was also suffering from “ventricular tachycardia.” He was then told to slap the defibrillator pads to his chest. They first elected to give him an antidote for the digoxin, but it was ineffective, so they proceeded to radio James and instructed him to defibrillate himself. James tries on multiple occasions to deliver the shock unsuccessfully, only to discover one of the connection pins to the defibrillator pads had become unplugged. He loses consciousness before he can replace the pin and collapses in the front seat of his car. Fortunately, his new-found love interest, Vesper Lynd (french actress Eva “OMG” Green), found James, plugged in the pin and proceed to cardiovert poor James back to life. As is true with Hollywood, he awakens unscathed and returns to the poker table, only to tell his arch rival Le Chiffre, “That last hand nearly killed me.”
Classic Bond. Great entertainment. Just a bit unreal, but then again, who wants reality when you can have "Bond,…
… James Bond."
-Wes
Device-based Hypertension Therapy?
All of us have had our blood pressure taken when we visit the doctor's office. Many of us have been told by a doctor that our blood pressure is too high and that we should "watch" it. Few of us, however, leave the doctor's office understanding how serious a health problem high blood pressure is or that it can lead to heart disease, stroke and kidney failure.
It is not that high blood pressure is especially difficult to control. Today's doctors can prescribe a wide range of good, affordable drugs that will lower your blood pressure and help you live a longer, healthier life. The problem is many of them simply don't. Some estimates have suggested that only 30-47% of patients with hypertension receive adequate therapy.
But occasionally, even with lots of medications and careful follow-up, there are a few patients in whom controlling blood pressure can be particularly difficult. For these patients there might be another option soon.
A new pacemaker-like device recently debuted at the American Heart Association meeting in Chicago this year to treat severe, drug–refractory hypertension. Made by CVRx, this device functions by stimulating the carotid bulb at the bifurcation (branch point) of the internal and external carotid arteries to activate the baroreceptor reflex.
The baroreceptor reflex is a normal reflex that the body uses to quickly provide more or less blood pressure to the brain with changes in posture. Elevation in blood pressures causes mechanical stretch of receptors (“baroreceptors”) in the carotid sinus. When stretched, these cells fire electrical impulses faster to stimulate centers in the brain that are responsible for deactivating sympathetic stimuli while activating the parasympathetic (or heart rate slowing and vasodilating portion of the body’s blood-pressure-regulating system to lower blood pressure. By stimulating these baroreceptors, researchers hope to use the body’s own baroreceptor reflex to drive blood pressure lower. The report of piloted patients appeared promising enough for the Food and Drug Administration to grant an Investigational Device Exemption (IDE) to expand the evaluation of the device to a larger cohort of patients.

Figure from the CVRx website
Early European results were reported for 12 patients at the European Society of Hypertension meeting in June 2006. In this study, after three months of active therapy, systolic blood pressure was reduced by an average of 24 mmHg (189 mmHg vs. 165 mmHg). In the preliminary US trial presented at the AHA meeting, three months of active therapy reduced systolic blood pressure by an average of 22 mmHg (180 mmHg vs. 158 mmHg) and diastolic blood pressure by an average of 18 mmHg (105 mmHg vs. 87 mmHg), using office cuff measurements. While data are preliminary at present, this device might become promising.
But there are some significant hurdles for the company to clear before the device can become reality.
First, because hypertension is painless and causes no symptoms until end-organ damage occurs, treating patients with an implantable device will be a hard sell for physicians. Furthermore, many patients with hypertension are simply left untreated by their physicians, or receive inadequate medical therapy. Confounding social and psychological problems, like alcoholism and medication non-compliance, further complicate therapy of hypertension. To think that such cases of hypertension warrant therapy with an implantable device is misguided.
Vanity, as well, will be difficult to overcome. From my experience with pacemakers, patients do not like their scar and associated discomfort occasionally experienced from pacemaker implantation beneath the collar bone (clavicle). Fortunately a shirt can usually cover the scar. But will patients want scars on both side of their neck with this device?
Safety issues also need to be addressed more completely. If the device is too effective in an individual patient and drop their blood pressure precipitously, how will it be inhibited? No sensor exists in the device to sense its effects on a persons’ blood pressure – certainly this is not a minor issue. Further, the baroreflex can cause profound slowing of the heart rate, or even asystole (no heart rate). No mechanism for pacing the heart (or a means of sensing the patient’s heart rate) exists in the device’s current design should a slow heart rhythm occur.
Finally, I hope that patients with renovascular hypertension are sufficiently screened before enrolling in a study using this device. Blocked arteries leading to the kidneys can result in profound medically-refractory blood pressure elevations and should be excluded before implanting this device.
In summary, the concept is interesting, but significant refinements are required before this device reaches the broader public. For now, treating hypertension early and often with conventional medical therapy and careful counselling is much more likely to be cost-effective at stemming hypertension’s end-organ complications.
-Wes
It is not that high blood pressure is especially difficult to control. Today's doctors can prescribe a wide range of good, affordable drugs that will lower your blood pressure and help you live a longer, healthier life. The problem is many of them simply don't. Some estimates have suggested that only 30-47% of patients with hypertension receive adequate therapy.
But occasionally, even with lots of medications and careful follow-up, there are a few patients in whom controlling blood pressure can be particularly difficult. For these patients there might be another option soon.
A new pacemaker-like device recently debuted at the American Heart Association meeting in Chicago this year to treat severe, drug–refractory hypertension. Made by CVRx, this device functions by stimulating the carotid bulb at the bifurcation (branch point) of the internal and external carotid arteries to activate the baroreceptor reflex.
The baroreceptor reflex is a normal reflex that the body uses to quickly provide more or less blood pressure to the brain with changes in posture. Elevation in blood pressures causes mechanical stretch of receptors (“baroreceptors”) in the carotid sinus. When stretched, these cells fire electrical impulses faster to stimulate centers in the brain that are responsible for deactivating sympathetic stimuli while activating the parasympathetic (or heart rate slowing and vasodilating portion of the body’s blood-pressure-regulating system to lower blood pressure. By stimulating these baroreceptors, researchers hope to use the body’s own baroreceptor reflex to drive blood pressure lower. The report of piloted patients appeared promising enough for the Food and Drug Administration to grant an Investigational Device Exemption (IDE) to expand the evaluation of the device to a larger cohort of patients.

Early European results were reported for 12 patients at the European Society of Hypertension meeting in June 2006. In this study, after three months of active therapy, systolic blood pressure was reduced by an average of 24 mmHg (189 mmHg vs. 165 mmHg). In the preliminary US trial presented at the AHA meeting, three months of active therapy reduced systolic blood pressure by an average of 22 mmHg (180 mmHg vs. 158 mmHg) and diastolic blood pressure by an average of 18 mmHg (105 mmHg vs. 87 mmHg), using office cuff measurements. While data are preliminary at present, this device might become promising.
But there are some significant hurdles for the company to clear before the device can become reality.
First, because hypertension is painless and causes no symptoms until end-organ damage occurs, treating patients with an implantable device will be a hard sell for physicians. Furthermore, many patients with hypertension are simply left untreated by their physicians, or receive inadequate medical therapy. Confounding social and psychological problems, like alcoholism and medication non-compliance, further complicate therapy of hypertension. To think that such cases of hypertension warrant therapy with an implantable device is misguided.
Vanity, as well, will be difficult to overcome. From my experience with pacemakers, patients do not like their scar and associated discomfort occasionally experienced from pacemaker implantation beneath the collar bone (clavicle). Fortunately a shirt can usually cover the scar. But will patients want scars on both side of their neck with this device?
Safety issues also need to be addressed more completely. If the device is too effective in an individual patient and drop their blood pressure precipitously, how will it be inhibited? No sensor exists in the device to sense its effects on a persons’ blood pressure – certainly this is not a minor issue. Further, the baroreflex can cause profound slowing of the heart rate, or even asystole (no heart rate). No mechanism for pacing the heart (or a means of sensing the patient’s heart rate) exists in the device’s current design should a slow heart rhythm occur.
Finally, I hope that patients with renovascular hypertension are sufficiently screened before enrolling in a study using this device. Blocked arteries leading to the kidneys can result in profound medically-refractory blood pressure elevations and should be excluded before implanting this device.
In summary, the concept is interesting, but significant refinements are required before this device reaches the broader public. For now, treating hypertension early and often with conventional medical therapy and careful counselling is much more likely to be cost-effective at stemming hypertension’s end-organ complications.
-Wes
Thursday, November 23, 2006
The Quiet Before the Storm
Wednesday, November 22, 2006
From My Wife for Thanksgiving
From my wife, for whom I am infinitely thankful:
At the beginning of the holiday season, our extended family is about to sit at the Thanksgiving table. This time, at an assisted living facility, where other hands will be cooking the meal, in a room rented for the family to gather. As I look around the table tomorrow, my blessing will be realizing how rare it is that we are able to have so many loved ones in one place at one time – if just for an imperfect, fractious moment. Young, some home from college, some zooming through puberty. Old, some on the brink of hospice, some befuddled and tired, but still here. There will be sports jerseys and size 14 shoes, cheeks sprinkled with acne, gorgeous young girls with straightened hair, others bending over a wheelchair, and middle-agers. Many of us have traveled across several states to be here. What a rare moment, before the great wheel of life turns again.
We have met for years exactly like this (but in someone’s home), but this year I seem to understand the fleetingness of our time with each other. The young adults will move on, and so will the old. Some at the table have thus far led a blessed life – untouched by any misfortune. Others, including some of the young ones, have struggled with life-threatening illnesses and chronic disease, crippling depression and stunning failures. We join in all our imperfection, our silliness and preoccupation, our greatness and growing wisdom. If we are lucky, we sit at the Thanksgiving table able to give true thanks, albeit for a life that we barely understand. I hope you can too.
-Diane
At the beginning of the holiday season, our extended family is about to sit at the Thanksgiving table. This time, at an assisted living facility, where other hands will be cooking the meal, in a room rented for the family to gather. As I look around the table tomorrow, my blessing will be realizing how rare it is that we are able to have so many loved ones in one place at one time – if just for an imperfect, fractious moment. Young, some home from college, some zooming through puberty. Old, some on the brink of hospice, some befuddled and tired, but still here. There will be sports jerseys and size 14 shoes, cheeks sprinkled with acne, gorgeous young girls with straightened hair, others bending over a wheelchair, and middle-agers. Many of us have traveled across several states to be here. What a rare moment, before the great wheel of life turns again.
We have met for years exactly like this (but in someone’s home), but this year I seem to understand the fleetingness of our time with each other. The young adults will move on, and so will the old. Some at the table have thus far led a blessed life – untouched by any misfortune. Others, including some of the young ones, have struggled with life-threatening illnesses and chronic disease, crippling depression and stunning failures. We join in all our imperfection, our silliness and preoccupation, our greatness and growing wisdom. If we are lucky, we sit at the Thanksgiving table able to give true thanks, albeit for a life that we barely understand. I hope you can too.
-Diane
Thanksgiving
As relatives arrive and meals are prepared for the traditional Thanksgiving observance here in the United States, it is useful to reflect back to the original observance credited to a gathering of Pilgrims and the Wampanoag Native Americans. Theirs was a celebration of post-harvest fortunes in 1621. The celebration occurred because of an unusually abundant harvest that year. Other years had not been so fortunate, since the number of Native Americans exceeded the number of surviving English at that point – a point often forgotten in the remembrance of this day.
Life was difficult then. Disease was common. Life expectancy to a child born in 1621, was a mere 35 years: nowhere near what we enjoy now. And while each of us should reflect and give thanks for our friends, family, and material goods we have today, perhaps the greatest gift that we can give thanks for is our longevity and the additional time we have to live our lives together.
It is remarkable to remember that penicillin wasn’t discovered by Alexander Fleming until 1928 and has ushered in the remarkable antibiotic era we enjoy today. That is only 78 years ago: about one man’s lifetime today. But in 1928, penicillin was cleared so quickly by the kidneys that it was often recaptured and purified from a patient’s urine due to short supply of the drug. Gratefully, probenecid was later developed to slow penicillin’s excretion in the kidneys. And more developments soon followed. Development after rapid development. The number of antibiotics available today is staggering.
Eric Zorn, a syndicated columnist from the Chicago Tribune today, put it this way:
So as you sit down for a holiday meal, stop, think, reflect, and give thanks…
… for life.
-Wes
Life was difficult then. Disease was common. Life expectancy to a child born in 1621, was a mere 35 years: nowhere near what we enjoy now. And while each of us should reflect and give thanks for our friends, family, and material goods we have today, perhaps the greatest gift that we can give thanks for is our longevity and the additional time we have to live our lives together.
It is remarkable to remember that penicillin wasn’t discovered by Alexander Fleming until 1928 and has ushered in the remarkable antibiotic era we enjoy today. That is only 78 years ago: about one man’s lifetime today. But in 1928, penicillin was cleared so quickly by the kidneys that it was often recaptured and purified from a patient’s urine due to short supply of the drug. Gratefully, probenecid was later developed to slow penicillin’s excretion in the kidneys. And more developments soon followed. Development after rapid development. The number of antibiotics available today is staggering.
Eric Zorn, a syndicated columnist from the Chicago Tribune today, put it this way:
At my age 600 years ago, even if I were Eric I of England, I’d likely be reposing in a splendid crypt. As it is, I’m perfectly healthy and taking the kids to see their grandmother in Pittsburgh, entertaining them in the mini-van with a tiny electronic slab that holds 1,500 songs, eight podcasts and two unabridged books on tape.Yes, he’s solidly, and remarkably, in “mid-life” with plenty of years still ahead.
So as you sit down for a holiday meal, stop, think, reflect, and give thanks…
… for life.
-Wes
Tuesday, November 21, 2006
Medical Blogging Grand Rounds 3.09 is Up!
The best of Medical Blogging Grand Rounds is up at Dr. Anonymous. It's a job very, very well done.
-Wes
-Wes
Monday, November 20, 2006
Holidays on "ICE"

Today, I learned about MedicAlert bracelets being offered to all children in Canada for free. For those unfamiliar with the MedicAlert bracelets, these are handy bracelets or necklaces used to notify Emergency or law enforcement personnel about important medical conditions or allergies in the event of an emergency. The bracelet contains relevant medical information on the "dog-tag" like necklace or bracelet. The only problem with these is that once they are printed, they are tough to modify. To counter this, they now have a MedicAlert "E-Health Key" (basically a USB thumb drive) which has been introduced that can carry much more information that can be modified on one's computer. For an annual fee, there is also a 24-hour service to notify EMS and law enforcement vital medical information or your family. We have historically encouraged our patients with pacemakers and defibrillators, or those on anticoagulation medications like warfarin (Coumadin), to have one of these. But now, we also might offer another suggestion.
What I'm thinking about is making sure every puts their Holidays (and Cell Phones) on "ICE." No, I'm not suggesting everyone go out and buy the new David Sedaris book by the same title as this post (although it is a funny read about dysfunctional families at holiday time). No, it's much more practical and virtually free.
With the near ubiquitous availability of cell phone's in many of today's children and adults (at least in much of the US), a similar readily-available means of medical information and contact information could also be achieved using an entry called "ICE," In Case of Emergency, on your child or loved one's cell phone. Enter your number for emergency contact information, and under, say, "ICE-2" you could place your child's allergies and under "ICE-3" your child's medications. With the cell phone idea, your information can be easily updated, and will not cost additional money and ER personnel are making it a habit to check the phone's address book for an ICE entry.
So if you don't register for a MedicAlert bracelet and notification service, consider updating your cell phone today. It could just save a life - even yours.
-Wes
For disclosure, I have no conflict of interest with Amazon, MedicAlert services or products, or David Sedaris.
Sunday, November 19, 2006
Cool Infect-o-Meter
I wish I had thought of this.
Pulse oximeters, devices that measure the oxygen level in a person's blood non-invasively in real-time, use the same technology. Only problem is, if no blood is reaching the wound to promote wound healing, no antibiotics will either. But the potential of this device to urge doctors to intervene earlier with treatment during wound healing is intriguing.
-Wes
Pulse oximeters, devices that measure the oxygen level in a person's blood non-invasively in real-time, use the same technology. Only problem is, if no blood is reaching the wound to promote wound healing, no antibiotics will either. But the potential of this device to urge doctors to intervene earlier with treatment during wound healing is intriguing.
-Wes
Saturday, November 18, 2006
On Schembechler's Death: Explant His Device?
I read the press reports of Mr. Schembechler’s death this morning (WSJ):
I think his death, like many others that we’re less likely to hear about, illustrates my earlier point about letting people die in peace. The recent call to explant all medical devices (pacemakers and defibrillators), like rushing to a airplane crash to look for the black box flight recorder to see what actually caused the demise of an individual, might not be appropriate in most circumstances. Mr. Schembechler had a long history of cardiac disease. People with severe heart disease die from heart rhythm disturbances and pump failure. Yes, some die from cardiac device malfunctions, but these are decidedly rare. There are those that feel that explanting every device and returning it to the manufacturer will improve quality products in the future. Perhaps. But once we embark on this tract, the potential to exacerbate the liability mess in medicine seems inevitable.
Let’s say (only conjecture here), that Mr. Schembechler’s “pacemaker” device was later explanted. Three months later the manufacturing company concludes that the "root cause" of the device malfunction was cosmic radiation that caused a short-circuit in a chip on his device. Certainly, there might be a later improvement in the manufacturing process to avoid a future problem. But should the family be informed that the reason their loved one died was the device? Who will notify them? Industry? One of Mr. Schembechler’s physicians?
I can hear the lawyers salivating, can’t you?
-Wes
Bo Schembechler, who became one of college football's great coaches in two decades at Michigan, died Friday after taping a TV show on the eve of the Wolverines' No. 1 vs. No. 2 showdown with perennial rival Ohio State. He was 77.First, let me say that I do not know the type of “pacemaker” device Mr. Schembechler received. Was it a "pacemaker" or "defibrillator?" The press rarely differentiate between these two “pacemaker-like” devices. (Defibrillators detect and treat rapid and slow cardiac rhythms while pacemakers just support slow cardiac rhythms). I don’t consider the age of 77 to be that old anymore and would likely have implanted a “defibrillator” rather than a pacemaker, given the degree of cardiac disease Mr. Schembechler suffered from. But this misses my central point today.
Mr. Schembechler collapsed at the studios at WXYZ-TV in the Detroit suburb of Southfield and was taken by ambulance to a nearby hospital. His death at 11:42 a.m. was confirmed by Mike Dowd, chief investigator for the medical examiner's office in Oakland County.
"It was probably not a heart attack; it just stopped working," Shukri David said.
Mr. Schembechler had a heart attack on the eve of his first Rose Bowl in 1970 and another one in 1987. He had two quadruple heart-bypass operations, and doctors implanted a pacemaker to regulate his heartbeat after he became ill during a taping at WXYZ on Oct. 20.
I think his death, like many others that we’re less likely to hear about, illustrates my earlier point about letting people die in peace. The recent call to explant all medical devices (pacemakers and defibrillators), like rushing to a airplane crash to look for the black box flight recorder to see what actually caused the demise of an individual, might not be appropriate in most circumstances. Mr. Schembechler had a long history of cardiac disease. People with severe heart disease die from heart rhythm disturbances and pump failure. Yes, some die from cardiac device malfunctions, but these are decidedly rare. There are those that feel that explanting every device and returning it to the manufacturer will improve quality products in the future. Perhaps. But once we embark on this tract, the potential to exacerbate the liability mess in medicine seems inevitable.
Let’s say (only conjecture here), that Mr. Schembechler’s “pacemaker” device was later explanted. Three months later the manufacturing company concludes that the "root cause" of the device malfunction was cosmic radiation that caused a short-circuit in a chip on his device. Certainly, there might be a later improvement in the manufacturing process to avoid a future problem. But should the family be informed that the reason their loved one died was the device? Who will notify them? Industry? One of Mr. Schembechler’s physicians?
I can hear the lawyers salivating, can’t you?
-Wes
Friday, November 17, 2006
Turkey Bowling
I looked in the room and there he was. Sitting up slumped forward in his wheelchair, a slight temporal wasting to his brow. I knocked. His head raised and he seemed happy to see me. His arthritic joints reached the arms of the wheelchair to adjust his posture.
“How was your day?” he asked, smiling.
“Fine. How about you?”
“I’m tired, but these folks are wonderful. They seem to have a real purpose up here on rehab – they really seem to have the common goal of getting you ready to go home.”
Then I spied a tiny gold trophy cup on his bedside table. On the outside it said: “Turkey Bowling Champion – First Place”
“What’s this?”
“Oh, it’s nothing,” he chuckled, somewhat embarrassed by the trophy. “It really was pretty funny.”
“How so?”
“Well, I was asked if I wanted to turkey bowl with some others on the ward. Now I had no idea what the heck this was, but it the staff here were really talking it up. Anyway, the next thing I knew, there I was with three other ladies, all older than me, each in our wheelchairs. What a pitiful site!
They came over and handed me a four-pound frozen turkey with a little handle on it. On the other side of the room they had arranged some bowling pins. Each of us got a chance to try to knock those damn pins down. None of us could walk, but we just swung our arms back and forth, back and forth, and then let ‘er go. I had those pins right in my site, but the damn turkey doesn't roll very true, you know…
Well the ladies, they were winning at first…”
“How many frames did you play?”
“Oh, about six or seven. Those nice kids would run down and set up the pins after we’d chuck that thing toward them. It took me a while to get used to it.”
“So what happened?”
“Damn if I didn’t get a strike in the last frame! I won, but It was all random you know. The way that thing rolls any one of us could have won. If you had told me that I would be sitting here turkey bowling three weeks ago, I never would have believed it.”
I wouldn't have believed it either.
I now have a newfound respect and appreciation for physical therapists and occupational therapists. Relearning the little things, like standing safely, controlled breathing as you walk, planning ambulation strategies - it's all new to someone bedridden for a month. Words of encouragement, a helpful hand, and gentle coaxing, with a little "turkey bowling" thrown in, are sure to help anyone get moving again - it is a special gift, indeed.
Now I can’t wait for the rest of the family to arrive at Thanksgiving so we can practice for the next match...
-Wes
“How was your day?” he asked, smiling.
“Fine. How about you?”
“I’m tired, but these folks are wonderful. They seem to have a real purpose up here on rehab – they really seem to have the common goal of getting you ready to go home.”
Then I spied a tiny gold trophy cup on his bedside table. On the outside it said: “Turkey Bowling Champion – First Place”
“What’s this?”
“Oh, it’s nothing,” he chuckled, somewhat embarrassed by the trophy. “It really was pretty funny.”
“How so?”
“Well, I was asked if I wanted to turkey bowl with some others on the ward. Now I had no idea what the heck this was, but it the staff here were really talking it up. Anyway, the next thing I knew, there I was with three other ladies, all older than me, each in our wheelchairs. What a pitiful site!
They came over and handed me a four-pound frozen turkey with a little handle on it. On the other side of the room they had arranged some bowling pins. Each of us got a chance to try to knock those damn pins down. None of us could walk, but we just swung our arms back and forth, back and forth, and then let ‘er go. I had those pins right in my site, but the damn turkey doesn't roll very true, you know…
Well the ladies, they were winning at first…”
“How many frames did you play?”
“Oh, about six or seven. Those nice kids would run down and set up the pins after we’d chuck that thing toward them. It took me a while to get used to it.”
“So what happened?”
“Damn if I didn’t get a strike in the last frame! I won, but It was all random you know. The way that thing rolls any one of us could have won. If you had told me that I would be sitting here turkey bowling three weeks ago, I never would have believed it.”
I wouldn't have believed it either.
I now have a newfound respect and appreciation for physical therapists and occupational therapists. Relearning the little things, like standing safely, controlled breathing as you walk, planning ambulation strategies - it's all new to someone bedridden for a month. Words of encouragement, a helpful hand, and gentle coaxing, with a little "turkey bowling" thrown in, are sure to help anyone get moving again - it is a special gift, indeed.
Now I can’t wait for the rest of the family to arrive at Thanksgiving so we can practice for the next match...
-Wes
Thursday, November 16, 2006
Pushing the Envelope of Atrial Fibrillation Ablation
A preliminary, pilot, very small, study of 77 patients randomized between primary pulmonary vein isolation versus biventricular pacing with AV junctional ablation was reported at the American Heart Association meeting yesterday. Remarkable “success” was reported with atrial fibrillation ablation compared to the "ablate and pace" approach. But this physician urges caution in interpreting these results.
90% success rates for atrial fibrillation ablation, especially in patients with heart failure is decidedly unusual in the world’s literature. Could there be a bias in their selection of patients or reporting? The data need to be peer-reviewed. Further, anyone who has performed these procedures understands the difficulty performing this procedure from a technical standpoint. Heart failure patients usually have multiple co-morbidities and are at increased risk of complications. Nowhere in this press release were complications reported. Spending 3-5 hours in the left atrium of patients performing these procedures is a big deal for the patient, I believe, compared to implanting a biventricular pacemaker and performing a AV junctional ablation. Furthermore, the procedural preparation time before and follow-up after these atrial fibrillation procedures is considerable. I am aware that the Cleveland Clinic employs eight full time advanced practice nurses to answer between 50 and 100 telephone calls per day from their atrial fibrillation patients – hence these data may not be easily transferable to lower-volume centers.
While I appreciate the novelty of addressing heart failure with atrial fibrillation ablation procedures, patients and physicians alike need to view these data cautiously.
-Wes
90% success rates for atrial fibrillation ablation, especially in patients with heart failure is decidedly unusual in the world’s literature. Could there be a bias in their selection of patients or reporting? The data need to be peer-reviewed. Further, anyone who has performed these procedures understands the difficulty performing this procedure from a technical standpoint. Heart failure patients usually have multiple co-morbidities and are at increased risk of complications. Nowhere in this press release were complications reported. Spending 3-5 hours in the left atrium of patients performing these procedures is a big deal for the patient, I believe, compared to implanting a biventricular pacemaker and performing a AV junctional ablation. Furthermore, the procedural preparation time before and follow-up after these atrial fibrillation procedures is considerable. I am aware that the Cleveland Clinic employs eight full time advanced practice nurses to answer between 50 and 100 telephone calls per day from their atrial fibrillation patients – hence these data may not be easily transferable to lower-volume centers.
While I appreciate the novelty of addressing heart failure with atrial fibrillation ablation procedures, patients and physicians alike need to view these data cautiously.
-Wes
Uterine Tissue Factories
Imagine growing artifical heart valves in utero from stem cells floating about in amniotic fluid within the womb. Incredible? Or what about artificial bladders or blood vessels. Well, it has been done. Reported yesterday at the American Heart Association meeting:
And millions will be better for it.
-Wes
Scientists for the first time have grown human heart valves using stem cells from the fluid that cushions babies in the womb -- offering a revolutionary approach that may be used to repair defective hearts in the future.The era of stem cell therapy is here. Little uterine tissue factories will soon the churning throughout the globe. Perhaps not first in humans. No, it will probably be done in dogs or rabbits first:
The idea is to create new valves in the lab while the pregnancy progresses and have them ready to implant in a baby with heart defects after it is born.
The Swiss experiment follows recent success growing bladders and blood vessels and suggests people may one day be able to grow their own replacement heart parts -- in some cases, before they're born.
...Japanese researchers said they had grown new heart valves in rabbits using cells from the animals' own tissue. It is the first time replacement heart valves have been created in this manner, said lead author Dr. Kyoko Hayashida.But it's just a matter of time.
And millions will be better for it.
-Wes
Wednesday, November 15, 2006
Medicaid HMOs: Dump 'Em
Every wonder how Medicaid HMO's like WellCare, Centene Corporation, Molina Healthcare and Amerigroup Corporation can make so much money? Me too. But their profits have been so impressive that they're "giving back" to their communities and to politicians, even when most of their clients can't afford health care. From this morning's Wall Street Journal:
Maybe then they'll get the message: patients come first, before communities and before politicians.
-Wes
Centene last year was the biggest donor for a $9.5 million renovation of an arts building in St. Louis, now called the Centene Center for Arts and Education, according to a spokeswoman for the center. The company paid $200,000 last year for the naming rights of a minor-league baseball stadium in Montana, where Centene employs 100 claims processors but doesn't have Medicaid clients. Centene also pledged $400,000 this year to the school district in Clayton, Mo., where the company has its headquarters, to rename the district's stadium.Could it possibly be because they are not health care insurance providers but health care insurance deniers? After all, Medicaid HMOs, like other HMOs, seek to save money by eliminating unnecessary care and paying for preventive treatments. But who is deciding what amounts to "unnecessary care?"
Kuldeep Singh, an internist in Valdosta, Ga., says that when Georgia began to move more than a million Medicaid recipients into HMOs this year, he suddenly faced hurdles not imposed by regular Medicaid. Recently, he says, one of his assistants had to wait on hold to get approval from WellCare for a hospital chest X-ray on a patient suspected of having pneumonia. "It was ridiculous," says Dr. Singh. A spokesman for WellCare says it sometimes requires such approval because hospital-based X-rays cost two to three times as much as those done in a doctor's office or imaging center.Oh, I get it, take a sick, coughing person from a hospital to a doc-in-the-box. Brilliant, just brilliant. At least our state has caught on:
In Illinois, the state and the Justice Department asserted in a lawsuit that Amerigroup spent only $131 million on medical care from 2000 to 2004 despite taking in $243 million from the state. The lawsuit accused Amerigroup of fraudulently trying to exclude pregnant and sick patients to reduce its medical costs. A jury in Illinois state court agreed last month, finding Amerigroup liable to the government for $144 million. Internal Amerigroup emails filed in court show managers contemplated disciplinary action for employees who signed up women in the third trimester.It doesn't take a rocket scientist to figure out these guys are bilking our health care system. It's time to dump 'em.
Maybe then they'll get the message: patients come first, before communities and before politicians.
-Wes
Tuesday, November 14, 2006
Still Smoking?
It's time to quit. It's the best thing you'll ever do for yourself and family.
Oh, and put that $4 per pack away in the bank instead - you'll be about $1500 richer by the end of the year, good enough to buy yourself one of these.
-Wes
Oh, and put that $4 per pack away in the bank instead - you'll be about $1500 richer by the end of the year, good enough to buy yourself one of these.
-Wes
Monday, November 13, 2006
ICD Therapy: Oversold or Underutilized?
The debate on implantable cardiac defibrillators (ICDs) heated up today after a study was presented that reported on results of a survey of heart failure patients and their perceptions of the devices at the American Heart Association meeting here in Chicago. Turns out that patients believe their device is more likely to save their life than they actually do. The lead author, Dr. Lynne Warner Stevenson wants to make sure they know what they’re getting into if a device is implanted:
The crux of the argument is the difference between “relative risk reduction” and “absolute risk reduction.” “Relative” to patients without an ICD implanted, there were 23% fewer deaths compared to the non-ICD group in the SCD-HeFT trial, on which she based the above data. In “absolute” terms, if 100 patients were implanted, 7.1 fewer deaths occurred in the ICD-treated group than in the non-ICD treated group, all other things being equal.
Now, you’re the one with the crummy heart. A doctor leans forward and gives you the data. Which would you choose?
But to take this a bit further, Dr Stevenson added those other more questionable tidbits of data – I especially like the one that says “10-20 will have a shock when they don't need a shock.” Data regarding appropriate, life saving shocks were not mentioned. Why not? Here’s the REAL data from the New England Journal of Medicine publication:
829 patients received a single-lead ICD in the SCD-HeFT trial. From the NEJM paper:
The medical device industry is very concerned about the drop in ICD implantation rates recently. Industry is worried the recall fiasco is what caused their ICD implantation rates to plummet. I suggest this might not be the main reason. Instead, I think Dr. Stevenson has struck a cord regarding the real reason ICD implant rates have fallen (remember, Dr. Stephenson is a referring doctor). Referring doctors now know that ICD’s are not infallible, certainly, but more importantly, they realize the number of their patients that would have to be implanted to save one life: 12 to 15.
Is this too many? Too much cost? You decide.
It is what it is. But to avoid the issue in asymptomatic patients with weak heart muscles might result in tragedies, too. Coaches Maggie Dixon and Randy Walker come to mind. They looked good didn’t they? Hell, they were coaching.
This is tough to swallow, but given the effectiveness of ICD’s over drug therapy, we’d be fools to ignore the benefit of ICDs to our patients, all things considered. But certainly, being informed about their upsides and downsides in a balanced manner will go a long way toward helping our patients make this tough, life-long decision.
Now the tough question: if your patient can't decide, what would you recommend?
-Wes
"We now tell a patient that if we put an ICD in 100 patients with heart disease like yours, over the next five years we would expect 30 patients will die anyway, seven to eight will be saved by the ICD, 10-20 will have a shock when they don't need a shock, five to 15 will have other complications, and the rest of the patients will never experience a shock from their devices."Could this be true? Have we oversold these devices?
The crux of the argument is the difference between “relative risk reduction” and “absolute risk reduction.” “Relative” to patients without an ICD implanted, there were 23% fewer deaths compared to the non-ICD group in the SCD-HeFT trial, on which she based the above data. In “absolute” terms, if 100 patients were implanted, 7.1 fewer deaths occurred in the ICD-treated group than in the non-ICD treated group, all other things being equal.
Now, you’re the one with the crummy heart. A doctor leans forward and gives you the data. Which would you choose?
But to take this a bit further, Dr Stevenson added those other more questionable tidbits of data – I especially like the one that says “10-20 will have a shock when they don't need a shock.” Data regarding appropriate, life saving shocks were not mentioned. Why not? Here’s the REAL data from the New England Journal of Medicine publication:
829 patients received a single-lead ICD in the SCD-HeFT trial. From the NEJM paper:
Of the 829 patients in the ICD group, 259 (31 percent) were known to have received shocks from their device for any cause, with 177 (68 percent of the shocks, or 21 percent of the ICD group) receiving shocks for rapid ventricular tachycardia or fibrillation. During five years of follow-up, the average annual rate of ICD shocks was 7.5 percent. For appropriate shocks only (i.e., shocks for rapid, sustained ventricular tachycardia or fibrillation), the average annual rate of ICD shocks was 5.1 percent.So as I see it, using Dr. Stevenson’s analogy: of 100 patients, 7 to 8 patients will receive a shock each year with 5 or 6 of these patients receiving an appropriate shock, while 2 or 3 will have an inappropriate shock. Said another way, 2-3 patients over 5 years gives us about 10-15 patients getting inappropriate shocks, while 25 to 30 receive appropriate, potentially life-saving shocks over the same time period. The argument for an ICD sounds a bit stronger when you give both sides of the argument, doesn’t it?
The medical device industry is very concerned about the drop in ICD implantation rates recently. Industry is worried the recall fiasco is what caused their ICD implantation rates to plummet. I suggest this might not be the main reason. Instead, I think Dr. Stevenson has struck a cord regarding the real reason ICD implant rates have fallen (remember, Dr. Stephenson is a referring doctor). Referring doctors now know that ICD’s are not infallible, certainly, but more importantly, they realize the number of their patients that would have to be implanted to save one life: 12 to 15.
Is this too many? Too much cost? You decide.
It is what it is. But to avoid the issue in asymptomatic patients with weak heart muscles might result in tragedies, too. Coaches Maggie Dixon and Randy Walker come to mind. They looked good didn’t they? Hell, they were coaching.
This is tough to swallow, but given the effectiveness of ICD’s over drug therapy, we’d be fools to ignore the benefit of ICDs to our patients, all things considered. But certainly, being informed about their upsides and downsides in a balanced manner will go a long way toward helping our patients make this tough, life-long decision.
Now the tough question: if your patient can't decide, what would you recommend?
-Wes
Let Them Rest In Peace
Some think we should explant all defibrillators after people die so manufacturers can see how their devices performed. Given that 99.3-99.8% of all defibrillators function normally, I say let these poor people rest in peace after they die.
There's plenty companies can do to improve quality besides obtaining devices from mortuaries.
-Wes
There's plenty companies can do to improve quality besides obtaining devices from mortuaries.
-Wes
Door-to-Balloon Time: Simple?
You feel heaviness in your chest, throat tightening. You pop and aspirin and have your wife (or husband) take you to the Emergency Room. You've just hit the "door." The story is classic and the ER, fortunately, expedites your evaluation. An electrocardiogram is performed and demonstrates and acute myocardial infarction pattern: a heart attack is in progress. "Guys, call the cath lab," the ER attending pleads.
"Er, sir, it's one in the morning."
"Well, then, call the cardiologist and get them here... yesterday!"
Calls are made. Beepers activated. A cardiologist is roused from sleep, young technicians fumble for their pants and car keys. You hurt like hell, sweat pouring from your brow. Traffic laws are ignored. Red lites make an effective effort to stall. Time is ticking. Faster. Faster!
The cardiologist arrives first, meds are increased, your blood pressure drops. The techs arrive, switches activated. Lites turned on. X-ray system booted. Gown. Hat. Mask. Booties. Scrub. Trays opened. "Call the ER, tell 'em we're ready."
"Okay." The phone is dialed.
"Shit! They have no one to transport the patient! You go!" The tech runs to the lab. IV's hang from every corner of your bed. Doctors look concerned. Minutes. Tick. Hurry. "Get the elevator!" A nurse runs ahead to call the elevator. Tick. Tick. Tick. The door opens. Your bed is pushed into the elevator. You feel and IV yanked from your arm. "Hold it!" the tech screems. His IV pole wheel just got caught in the gap between the floor and the elevator. You feel a warm fluid near your elbow. "Damn it, hold pressure!" The fluid is blood. An IV fell out. Heparin. "We'll get another IV when we get to the lab. Don't worry about it." Go! Go! First floor, second floor. Ding! The elevator door opens. "Easy on the way out of the elevator. Okay, we're clear."
You're hurried to the lab down the hall. Once there, you enter a foreign room, lites blaring. AC/DC's "Hell's Bells" shreaks in the background." You're lifted to the narrowest table ever. Stickers are applied to your shoulders, prongs plugged in your nose, a clip applied to your finger. A big cold jelly-fish-like pad applied to your chest on each side. Pants removed. Warm, wet soap applied to your groins. You hear the scrub sink, with its water running, in the distance. Soon it stops. Another gown worn, another set of gloves applied.
"You're going to feel a little sting down here," the cardiologist says as the anesthetic is applied. Another sting is felt at your forearm."
"Ouch!" The cardiologist pauses. "Did that hurt?"
"Not down there, on my arm!"
"Sorry, I was starting another IV," the tech confesses. The cardiologist continues. The artery entered. A catheter passed to the heart. The coronary artery engaged and contrast administered. "That one's okay," the cardiologist thinks. "JL4 guider." Catheter are exchanged. More die injected, shots taken. The cardiologist turns away, working at the table as quickly as he can. A balloon is prepped, then inserted. "Whisper wire." The lesion is crossed. Your chest is heavier now. The balloon inflated, deflated. Suddenly, the pressure subsides. You relax. "How are you feeling now?"
"Better."
Door-to-balloon time. Simple in theory, yet not so simple in practice. Sweeping changes would have to be implemented in urban areas to achieve this. Techs and cardiologists, likely, would have to reside in-house when on call, or else live very close to their hospital, an impractical option in many cases. And while some recommendations by the American Heart Association and American College of Cardiology seem "simple" to some, their ramifications are significant to all. At least one doctor thinks this is a good idea:
While I do not argue that short door-to-balloon times save heart muscle, serious consideration of the costs to all involved, especially those doing the procedures, needs to be carefully examined. Presently we only get paid for doing the job - not waiting. The real people who are pushing this are the payors and hospitals. Why? Because patients do better, certainly, and costs fall. And their wallets swell.
But if "time is muscle," time waiting for a case is also lost money and personal lives to those doing the procedures.
So, who's gonna pay for all that waisted time?
The answer: Doctors.
-Wes
"Er, sir, it's one in the morning."
"Well, then, call the cardiologist and get them here... yesterday!"
Calls are made. Beepers activated. A cardiologist is roused from sleep, young technicians fumble for their pants and car keys. You hurt like hell, sweat pouring from your brow. Traffic laws are ignored. Red lites make an effective effort to stall. Time is ticking. Faster. Faster!
The cardiologist arrives first, meds are increased, your blood pressure drops. The techs arrive, switches activated. Lites turned on. X-ray system booted. Gown. Hat. Mask. Booties. Scrub. Trays opened. "Call the ER, tell 'em we're ready."
"Okay." The phone is dialed.
"Shit! They have no one to transport the patient! You go!" The tech runs to the lab. IV's hang from every corner of your bed. Doctors look concerned. Minutes. Tick. Hurry. "Get the elevator!" A nurse runs ahead to call the elevator. Tick. Tick. Tick. The door opens. Your bed is pushed into the elevator. You feel and IV yanked from your arm. "Hold it!" the tech screems. His IV pole wheel just got caught in the gap between the floor and the elevator. You feel a warm fluid near your elbow. "Damn it, hold pressure!" The fluid is blood. An IV fell out. Heparin. "We'll get another IV when we get to the lab. Don't worry about it." Go! Go! First floor, second floor. Ding! The elevator door opens. "Easy on the way out of the elevator. Okay, we're clear."
You're hurried to the lab down the hall. Once there, you enter a foreign room, lites blaring. AC/DC's "Hell's Bells" shreaks in the background." You're lifted to the narrowest table ever. Stickers are applied to your shoulders, prongs plugged in your nose, a clip applied to your finger. A big cold jelly-fish-like pad applied to your chest on each side. Pants removed. Warm, wet soap applied to your groins. You hear the scrub sink, with its water running, in the distance. Soon it stops. Another gown worn, another set of gloves applied.
"You're going to feel a little sting down here," the cardiologist says as the anesthetic is applied. Another sting is felt at your forearm."
"Ouch!" The cardiologist pauses. "Did that hurt?"
"Not down there, on my arm!"
"Sorry, I was starting another IV," the tech confesses. The cardiologist continues. The artery entered. A catheter passed to the heart. The coronary artery engaged and contrast administered. "That one's okay," the cardiologist thinks. "JL4 guider." Catheter are exchanged. More die injected, shots taken. The cardiologist turns away, working at the table as quickly as he can. A balloon is prepped, then inserted. "Whisper wire." The lesion is crossed. Your chest is heavier now. The balloon inflated, deflated. Suddenly, the pressure subsides. You relax. "How are you feeling now?"
"Better."
Door-to-balloon time. Simple in theory, yet not so simple in practice. Sweeping changes would have to be implemented in urban areas to achieve this. Techs and cardiologists, likely, would have to reside in-house when on call, or else live very close to their hospital, an impractical option in many cases. And while some recommendations by the American Heart Association and American College of Cardiology seem "simple" to some, their ramifications are significant to all. At least one doctor thinks this is a good idea:
"Thirty-five percent of patients in America have an artery opened in 90 minutes or less. Our goal is 75 percent," said Dr. Steven Nissen, president of the American College of Cardiology.Really? All physicians want this? All physicians want to live in the hospital waiting for that magic moment when an acute heart attack hits the door? How often does this happen? Five, maybe ten times a month? And how many occur after hours? Do all the techs want to live there waiting, too? Who will pay us for our time sitting, waiting?
"Everybody we've asked to do this has said this is the right thing to do. Payers want it. Government wants it. Hospitals want it. Physicians want it."
While I do not argue that short door-to-balloon times save heart muscle, serious consideration of the costs to all involved, especially those doing the procedures, needs to be carefully examined. Presently we only get paid for doing the job - not waiting. The real people who are pushing this are the payors and hospitals. Why? Because patients do better, certainly, and costs fall. And their wallets swell.
But if "time is muscle," time waiting for a case is also lost money and personal lives to those doing the procedures.
So, who's gonna pay for all that waisted time?
The answer: Doctors.
-Wes
Sunday, November 12, 2006
American Heart Meeting: First Impressions
With the tunes crankin', I drove down to the American Heart Association's Scientific Sessions today. On the way, the clouds parted a bit permitting a nice view of the city from the car down Lake Shore Drive ("Yes, officer, I was only traveling 60 MPH"):

The event was held at McCormick Place Convention Center. Huge is the operative word. Make sure you bring your hiking shoes! I often wonder if huge meetings like this are effective venues to really learn: I find I miss so much more than I can consume and as such, it's frustrating. But humans love social life and interacting with others, and this meeting certainly permits both. And for the advertisers, it's invaluable to have all of us doctor "consumers" packed in a (relatively) small space.
Upon entering from the Lakeside Conference Building (where indoor parking is located), you'll have to walk across the bridge spanning Lake Shore Drive South to the North and South Buildings:

(They tell be that guy at the lower right hand side of the picture went to Notre Dame. I wonder why they think that...) Anyway, if you stop at the top of the bridge and look to the North, you'll see the city's skyline. The stadium (Soldier Field) can be seen at the base of the skyline (the somewhat horizontal steel structure). Stand there in awe a moment and contemplate the Chicago Bears' season... then move on:

Once you cross the bridge, you'll enter the sea of humanity that is the AHA Meeting. I'm told it's a bit smaller than prior years, in part due to the attrition of most of the interventional cardiologists that now attend the Transcatheter Cardiovascular Therapeutics conference. Nonetheless, the scale of this meeting remains massive, and the attendance appears quite good this year.

The meeting begins in earnest tomorrow, with the first of the Late Breaking Clinical Trials being presented. It's a bit late to summarize the day, but perhaps I can spend some time tomorrow discussing our brief whirlwind tour of new devices on the horizon for heart failure therapies. Till then...
... good night!
-Wes

The event was held at McCormick Place Convention Center. Huge is the operative word. Make sure you bring your hiking shoes! I often wonder if huge meetings like this are effective venues to really learn: I find I miss so much more than I can consume and as such, it's frustrating. But humans love social life and interacting with others, and this meeting certainly permits both. And for the advertisers, it's invaluable to have all of us doctor "consumers" packed in a (relatively) small space.
Upon entering from the Lakeside Conference Building (where indoor parking is located), you'll have to walk across the bridge spanning Lake Shore Drive South to the North and South Buildings:

(They tell be that guy at the lower right hand side of the picture went to Notre Dame. I wonder why they think that...) Anyway, if you stop at the top of the bridge and look to the North, you'll see the city's skyline. The stadium (Soldier Field) can be seen at the base of the skyline (the somewhat horizontal steel structure). Stand there in awe a moment and contemplate the Chicago Bears' season... then move on:

Once you cross the bridge, you'll enter the sea of humanity that is the AHA Meeting. I'm told it's a bit smaller than prior years, in part due to the attrition of most of the interventional cardiologists that now attend the Transcatheter Cardiovascular Therapeutics conference. Nonetheless, the scale of this meeting remains massive, and the attendance appears quite good this year.

The meeting begins in earnest tomorrow, with the first of the Late Breaking Clinical Trials being presented. It's a bit late to summarize the day, but perhaps I can spend some time tomorrow discussing our brief whirlwind tour of new devices on the horizon for heart failure therapies. Till then...
... good night!
-Wes
Project Valor-IT Makes Its Goal
Congrats to the organizers of Project Valor-IT, who met (and exceeded) their goal of $180,000 toward voice-activated computer laptops for our injured troops. You can still give to this great cause here. I joined the Naval team.
-Wes
Hat-tip: Gruntdoc
-Wes
Hat-tip: Gruntdoc
Chicago Hosts AHA Scientific Sessions

Chicago certainly lived up to its moniker "The Windy City" two nights ago. O'Hare airport was closed to incoming air traffic as sustained winds of 40 MPH lashed our city and gusts to over 55 MPH were seen as our wonderful warm spell gave way to the Arctic blast thoroughly anchoring itself over the city. It's 40 degrees (Fahrenheit) and cloudy right now, but the winds have finally calmed - typical Chicago weather.
But what better venue than this for the American Heart Association's 2006 Annual Scientific Sessions? While fewer and fewer clinical cardiologists tend to attend this meeting, it remains the premiere meeting for basic scientists from around the world to share research interests and meet like-minded cardiovascular researchers in the areas of heart and vascular disease.
I will be attending this meeting later today and have even been invited to host a session tonight - even despite my rant about last year's local chapter meeting. I'll try to see if I can make a post or two about what I learn. It's a great chance to see old friends and learn about some of the latest research in heart disease.
Hope to see you there!
-Wes
Photo credit.
Friday, November 10, 2006
A 'Cool Case'
We’ve all had ‘em. No one wants to be one. Anyone in medicine long enough sees a cool case. Here's one of mine:
Years ago as a young electrophysiologist, I was asked to see a patient for consideration of an automatic defibrillator. He was a relatively young 49 year-old man who worked as a roofer and had a one-and-a-half year history of arthritis involving primarily his hands, elbows, and knees. He was treated with non-steroidal anti-inflammatory agents of all varieties without effect. He sought evaluation with a rheumatologist and was thought to have a form of non-rheumatic arthritis as his serologies were non-conclusive. He was eventually placed on a short course of steroids with some improvement, but his symptoms would return when the steroid dose was dropped. He eventually was required Plaquenil, a drug that can also suppress the immune system but served to help with the inflammation of his joints.
He had been in and out of the hospital on several occasions recently for increasing shortness of breath and rapid heart rhythms. His echocardiogram demonstrated a moderate weakening of his heart, and he had a mild elevation of his resting heart rate. His room-air oxygen level was lower than I would have expected. So he was treated with Lasix by the referring physician with some improvement. Because of his fairly poor heart function and rapid heart rhythms, we were consulted to evaluate him.
When I saw him he was short of breath, but able to lie flat with no more shortness of breath than usual. This was unusual for congestive heart failure. The remainder of his examination was only remarkable for bilateral basilar lung rales (crackles),
and the swollen, tender joints.
I examined his chest x-ray. It looked like this:
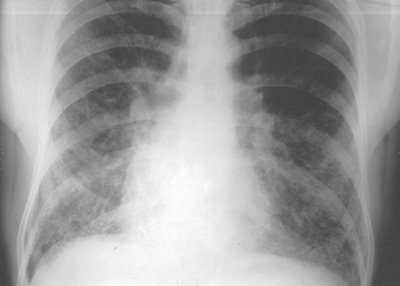
Now the fluffy infiltrative stuff in the lower lungs fields did NOT appear consistent with the usual causes of congestive heart failure that I had seen, so I thought I had better show the film to one of my pulmonary colleagues. He agreed with my interpretation and scheduled a bronchoscopy the next day, but later that day, he began coughing up blood. The procedure was expedited.
It was later that afternoon when the call came. "You're not going to believe this."
"What?"
And he proceeded to describe his findings on the bronchoscopy. Here's what he saw:

What did he find? (Click comments to see the answer).
-Wes
Years ago as a young electrophysiologist, I was asked to see a patient for consideration of an automatic defibrillator. He was a relatively young 49 year-old man who worked as a roofer and had a one-and-a-half year history of arthritis involving primarily his hands, elbows, and knees. He was treated with non-steroidal anti-inflammatory agents of all varieties without effect. He sought evaluation with a rheumatologist and was thought to have a form of non-rheumatic arthritis as his serologies were non-conclusive. He was eventually placed on a short course of steroids with some improvement, but his symptoms would return when the steroid dose was dropped. He eventually was required Plaquenil, a drug that can also suppress the immune system but served to help with the inflammation of his joints.
He had been in and out of the hospital on several occasions recently for increasing shortness of breath and rapid heart rhythms. His echocardiogram demonstrated a moderate weakening of his heart, and he had a mild elevation of his resting heart rate. His room-air oxygen level was lower than I would have expected. So he was treated with Lasix by the referring physician with some improvement. Because of his fairly poor heart function and rapid heart rhythms, we were consulted to evaluate him.
When I saw him he was short of breath, but able to lie flat with no more shortness of breath than usual. This was unusual for congestive heart failure. The remainder of his examination was only remarkable for bilateral basilar lung rales (crackles),
and the swollen, tender joints.
I examined his chest x-ray. It looked like this:

Now the fluffy infiltrative stuff in the lower lungs fields did NOT appear consistent with the usual causes of congestive heart failure that I had seen, so I thought I had better show the film to one of my pulmonary colleagues. He agreed with my interpretation and scheduled a bronchoscopy the next day, but later that day, he began coughing up blood. The procedure was expedited.
It was later that afternoon when the call came. "You're not going to believe this."
"What?"
And he proceeded to describe his findings on the bronchoscopy. Here's what he saw:

What did he find? (Click comments to see the answer).
-Wes
Device Programming Scam
I saw a case the other day that really disturbed me.
At first it seemed innocuous enough: a three-year old defibrillator whose battery was at end-of-life. But the battery voltage was unusually low: 1.59 volts. The elective replacement indicator (or “ERI,” as we call it) for this device was 2.51 volts.
Sometimes when battery voltages get real low, the devices don’t behave properly, so we elected to admit the patient and prep him/her (sex change for confidentiality reasons – you decide which gender you prefer to place in the sentence) for a battery change procedure.
While in the Electrophysiology Laboratory in a controlled setting, we checked the device, and were shocked to note that one of the leads was pacing at the maximum output of the device, but the pacing thresholds (the minimum voltage required to pace the heart) were much better than those settings. If the device had had its voltage dropped appropriately, battery voltage (and device longevity) could have been greatly preserved. The patient reassured me that he/she had been checked every three months while visiting another (undisclosed) state.
Now the potential explanations for this could be many: the person programming the device forgot to reset the lead voltage back to its appropriate setting, the threshold of the suspect lead actually DID improve (seems unlikely), the person programming the device wasn’t aware of the proper pacing threshold and wanted to “assure pacing,” or possibly as one of our local reps suggested (I hoped this was not the case), the doctor increased the voltage on the lead to burn out the battery faster so a new procedure would be needed sooner.
“Have you heard of this happening?” I asked the rep, who spoke on the condition of anonymity. After all, scores of engineers have worked tirelessly to develop algorithms (like St. Jude's Autocapture, or Medtronic's Capture Management and Search AV features) to preserve battery life and promote device longevity.
“Well, I’ve seen it. Usually not as dramatic as this, but voltages are increased to ‘assure safety’ but really they’re also interested in procedures,” he/she said.
Geez. How does one prove this if it is happening? There’s plenty of cover here: device reps often help busy doctors reprogram pacemakers (Device companies: can you say liability?). This leads to the “Gee, I didn’t know” syndrome to deflect liability. Could this be done “in the best interest of the patient” to assure pacing in those who are pacemaker-dependent for their hearts to beat? (Sounds noble, doesn’t it?) There seems to be no easy way to catch slimy physicians who might be involved in such a scheme. Patients need to be aware this could be happening and stay informed how their devices are programmed: ask for a copy of the interrogation of your device, my friends.
Fortunately, it appears that the FDA might have a way to thwart such behavior. There is a push at the FDA to develop powerful databases to monitor characteristics of implantable devices after they are approved to the public via large databases. Most of this is to assure product safety and reliability. But trends can be identified regarding implanters, as well. Scumbag physicians beware.
Additionally, the development of newer internet-capable medical devices that relay their programming information to a centralized database will permit the monitoring of trends to avoid such a programming “mistake” for patients, but doctors involved in the management of these patients need to remain vigilant for this potential scam.
-Wes
At first it seemed innocuous enough: a three-year old defibrillator whose battery was at end-of-life. But the battery voltage was unusually low: 1.59 volts. The elective replacement indicator (or “ERI,” as we call it) for this device was 2.51 volts.
Sometimes when battery voltages get real low, the devices don’t behave properly, so we elected to admit the patient and prep him/her (sex change for confidentiality reasons – you decide which gender you prefer to place in the sentence) for a battery change procedure.
While in the Electrophysiology Laboratory in a controlled setting, we checked the device, and were shocked to note that one of the leads was pacing at the maximum output of the device, but the pacing thresholds (the minimum voltage required to pace the heart) were much better than those settings. If the device had had its voltage dropped appropriately, battery voltage (and device longevity) could have been greatly preserved. The patient reassured me that he/she had been checked every three months while visiting another (undisclosed) state.
Now the potential explanations for this could be many: the person programming the device forgot to reset the lead voltage back to its appropriate setting, the threshold of the suspect lead actually DID improve (seems unlikely), the person programming the device wasn’t aware of the proper pacing threshold and wanted to “assure pacing,” or possibly as one of our local reps suggested (I hoped this was not the case), the doctor increased the voltage on the lead to burn out the battery faster so a new procedure would be needed sooner.
“Have you heard of this happening?” I asked the rep, who spoke on the condition of anonymity. After all, scores of engineers have worked tirelessly to develop algorithms (like St. Jude's Autocapture, or Medtronic's Capture Management and Search AV features) to preserve battery life and promote device longevity.
“Well, I’ve seen it. Usually not as dramatic as this, but voltages are increased to ‘assure safety’ but really they’re also interested in procedures,” he/she said.
Geez. How does one prove this if it is happening? There’s plenty of cover here: device reps often help busy doctors reprogram pacemakers (Device companies: can you say liability?). This leads to the “Gee, I didn’t know” syndrome to deflect liability. Could this be done “in the best interest of the patient” to assure pacing in those who are pacemaker-dependent for their hearts to beat? (Sounds noble, doesn’t it?) There seems to be no easy way to catch slimy physicians who might be involved in such a scheme. Patients need to be aware this could be happening and stay informed how their devices are programmed: ask for a copy of the interrogation of your device, my friends.
Fortunately, it appears that the FDA might have a way to thwart such behavior. There is a push at the FDA to develop powerful databases to monitor characteristics of implantable devices after they are approved to the public via large databases. Most of this is to assure product safety and reliability. But trends can be identified regarding implanters, as well. Scumbag physicians beware.
Additionally, the development of newer internet-capable medical devices that relay their programming information to a centralized database will permit the monitoring of trends to avoid such a programming “mistake” for patients, but doctors involved in the management of these patients need to remain vigilant for this potential scam.
-Wes
Thursday, November 09, 2006
Institute of Medicine's Big Error
Today's Wall Street Journal reports that Unitedhealth's chief executive William W. McGuire and his successor, Stephen J. Hemsley have agreed to pay back $390 million to Unitedhealth in an attempt to avoid "even the appearance of any unintended benefit from any past option grants." Of that amount, $200 million will come from Mr. McGuire - a fairly paltry portion (11.4%) of his $1.75 billion in total options issued. And worse still:
And what about the deficit that Mr. McGuire has caused to Unitedhealth's shareholders? If past history is any indication, anything where Mr. McGuire is "pleased to have reached an agreement" probably means he's still getting away with millions.
As such, should he really continue with the Institute of Medicine as a member of the National Institutes of Health National Cancer Policy Board? I suppose this is one medical error we'll never hear about from the Insititute of Medicine now will we?
-Wes
His attorney, David Brodsky, said, "Dr. McGuire is pleased to have reached an agreement to reprice his options. The agreement to forgo approximately $200 million means that Dr. McGuire will receive no benefit at all from dating issues in connection with his options."Earth to Mr. Brodsky: sounds like there's still some benefit in there to me.
But Dr. McGuire hasn't yet agreed to forfeit the reactivated options in which he and other employees were effectively able to get the same options twice, at favorable prices. For Dr. McGuire alone, those extra options are now valued at about $250 million. The issue of those options hasn't been resolved between Dr. McGuire and the company, according to people familiar with the situation.
And what about the deficit that Mr. McGuire has caused to Unitedhealth's shareholders? If past history is any indication, anything where Mr. McGuire is "pleased to have reached an agreement" probably means he's still getting away with millions.
As such, should he really continue with the Institute of Medicine as a member of the National Institutes of Health National Cancer Policy Board? I suppose this is one medical error we'll never hear about from the Insititute of Medicine now will we?
-Wes
Wednesday, November 08, 2006
Resurrecting Confidence
I visited Boston Scientific corporate headquarters yesterday trying to understand what they’re going to do to resurrect their business in the Cardiac Disease Management section of their company -- the Guidant portion of their business.
I met with a number of individuals: Mark Bartell, Senior VP, Global Sales and Marketing (tough job #1), a few of the heart failure marketing folks, Randy Ban, VP Marketing in charge of Corporate Communication Strategy, a fellow Dukie (go Blue Devils!) John Russell, who is in charge of the Latitude Patient Management System, and perhaps the most impressive person recruited to salvage the quality mess: Bill Young, VP of Reliability and Quality, a former Baxter quality professional with friends in high places at the FDA. This was a good pick as far as I can tell.
And why do you think I saw these particular individuals? Because they knew I am a skeptic. I have bright patients who read the newspapers and press reports. I have patients who say, “You can implant any device, except a Guidant device” when I tell them they need a defibrillator.
So what did I learn today?
In short: they’ve gotten the message.
They understand that a 99.2% or 99.3% device reliability is not good enough for the public and doctors, especially when you implant tens of thousands of these devices that must work years after they are implanted, charge hospitals and patients big bucks for them, and are withholding when problems with their devices surface. Like the airplane industry that has learned that it's not okay to have 1 in 1000 planes crash, I think they've made a good-faith effort to re-establish the importance of quality and long-term reliability in their products.
They also have learned that reporting failures TOO early can unnecessarily frighten patients, that doctors and the FDA can be helpful, that they’ve got more to do. All engines are geared right now to clearing their FDA 483 warning letter. They say they’re ready for their inspection, due any day. We’ll see. But they have changed personnel, recruited like crazy to shore up their quality and reliability shortcomings, and changed their corporate quality reporting structure to avoid internal conflicts of interest. Time will tell.
One of the best new standards they have implemented that can tangently be identified, was their online product performance reports. (Unfortunately it's still on their Guidant website - they really need to bury that name! But I digress.) Reportedly, this report is updated every three months. This, my friends, is impressive and welcomed. Now if a patient wonders about the reliability of a proposed implant, the information is quickly available on-line. This should be an industry standard.
And their marketing strategy? Lay low. Keep the old bad experiences out of the press. Look for plenty of “feel-good” pieces on Latitude, but also look for behind the scenes settling of their litigation burdens, which are considerable. Slowly. Quietly. Carefully.
Seems like a good plan. But all of this aside, it will mean nothing if they don't execute - and the raising of their FDA Warning Letter will be their first test.
-Wes
I met with a number of individuals: Mark Bartell, Senior VP, Global Sales and Marketing (tough job #1), a few of the heart failure marketing folks, Randy Ban, VP Marketing in charge of Corporate Communication Strategy, a fellow Dukie (go Blue Devils!) John Russell, who is in charge of the Latitude Patient Management System, and perhaps the most impressive person recruited to salvage the quality mess: Bill Young, VP of Reliability and Quality, a former Baxter quality professional with friends in high places at the FDA. This was a good pick as far as I can tell.
And why do you think I saw these particular individuals? Because they knew I am a skeptic. I have bright patients who read the newspapers and press reports. I have patients who say, “You can implant any device, except a Guidant device” when I tell them they need a defibrillator.
So what did I learn today?
In short: they’ve gotten the message.
They understand that a 99.2% or 99.3% device reliability is not good enough for the public and doctors, especially when you implant tens of thousands of these devices that must work years after they are implanted, charge hospitals and patients big bucks for them, and are withholding when problems with their devices surface. Like the airplane industry that has learned that it's not okay to have 1 in 1000 planes crash, I think they've made a good-faith effort to re-establish the importance of quality and long-term reliability in their products.
They also have learned that reporting failures TOO early can unnecessarily frighten patients, that doctors and the FDA can be helpful, that they’ve got more to do. All engines are geared right now to clearing their FDA 483 warning letter. They say they’re ready for their inspection, due any day. We’ll see. But they have changed personnel, recruited like crazy to shore up their quality and reliability shortcomings, and changed their corporate quality reporting structure to avoid internal conflicts of interest. Time will tell.
One of the best new standards they have implemented that can tangently be identified, was their online product performance reports. (Unfortunately it's still on their Guidant website - they really need to bury that name! But I digress.) Reportedly, this report is updated every three months. This, my friends, is impressive and welcomed. Now if a patient wonders about the reliability of a proposed implant, the information is quickly available on-line. This should be an industry standard.
And their marketing strategy? Lay low. Keep the old bad experiences out of the press. Look for plenty of “feel-good” pieces on Latitude, but also look for behind the scenes settling of their litigation burdens, which are considerable. Slowly. Quietly. Carefully.
Seems like a good plan. But all of this aside, it will mean nothing if they don't execute - and the raising of their FDA Warning Letter will be their first test.
-Wes
Hygenic Profiling
If you haven’t traveled recently on the airlines, be prepared. The planes are packed and often overbooked. Folks are asked to try a later flight, but the odds of getting on even later flights seem dim due to overbooking there, too. Heck, if the airlines aren’t making money now, they never will. Damn plane is packed with people. We’re sardines, one and all. There seem to be all kinds of nerds with that Bluetooth hands-free microphone thing strapped to their ear, shouting directions to their secretaries as we sit on the tarmac. Miserable. Now I know how these airlines have good on-time departures: they load everybody up, then pull over to an edge of the taxi-way, and shut down the engine.
“We’ve been notified that air traffic control has delayed our take-off. We’ll be here another hour, so you can use your cell phones.” Well, I chose to blog. I love my Treo.
A funny thing happened through the pre-flight screening. I had taken am opened implantable cardiac defibrillator in my bag. Here’s a picture of it:

Now it was amazing to me that this little device, with its battery, large capacitors that can charge to 800 volts, electronics, on-board computer... this would be ignored in a carry-on bag. Yep - went right through - no questions asked. But this, my friends, stopped traffic:

My trusty well-used toothpaste container placed in my zip-lock baggie: stopped, inspected, examined, delayed the line.
I am convinced this is “hygenic profiling.” You know, stopping to examine my toothpaste for no good reason. Poor toothpaste! Minding its own business, soaking up the xray radiation, and BAM! Some guy stops the conveyor belt to examine the contents while completely ignoring my defibrillator and its electronic contents.
Shows you what they're interested in these days...
Have fun at Thanksgiving time!
-Wes
“We’ve been notified that air traffic control has delayed our take-off. We’ll be here another hour, so you can use your cell phones.” Well, I chose to blog. I love my Treo.
A funny thing happened through the pre-flight screening. I had taken am opened implantable cardiac defibrillator in my bag. Here’s a picture of it:

Now it was amazing to me that this little device, with its battery, large capacitors that can charge to 800 volts, electronics, on-board computer... this would be ignored in a carry-on bag. Yep - went right through - no questions asked. But this, my friends, stopped traffic:

My trusty well-used toothpaste container placed in my zip-lock baggie: stopped, inspected, examined, delayed the line.
I am convinced this is “hygenic profiling.” You know, stopping to examine my toothpaste for no good reason. Poor toothpaste! Minding its own business, soaking up the xray radiation, and BAM! Some guy stops the conveyor belt to examine the contents while completely ignoring my defibrillator and its electronic contents.
Shows you what they're interested in these days...
Have fun at Thanksgiving time!
-Wes
Tuesday, November 07, 2006
Medical Grand Rounds Floats Your Boat While You Vote
The best of Medical Blogging this week can be found at Medical Staff Services Professionals Nexus Blog. Be sure your credentials packet is up to date, lest you be stopped in the halls...
From a Wall Street Journal/Harris Interactive Poll published 24 Oct 2006:
Let's try to make that 13% of folks not voting a bit smaller...
May your favorite candidate win!
-Wes
Before a surgeon's scalpel cuts open a patient, before a generalist signs a prescription, someone like Rita Schwab gets involved. She's a Medical Staff Service Professional and, simply put, MSSPs make the hospital run by verifying the credentials of its physicians and staff. Jobs like Schwab's are increasingly gaining prominence, in part due to today's risk-averse, more transparent hospital administrations, but also in part due to Web sites like MSSPnexus, Schwab's effort to reach out to colleagues and those who'd like to learn more about her role.But on the way, don't forget to vote today!
From a Wall Street Journal/Harris Interactive Poll published 24 Oct 2006:
| TOTAL | Republican | Democrat | Independent | |
| Healthcare Is an Important Issue (Sub-Net) | 68% | 66% | 81% | 69% |
| Healthcare will be the most important issue to me | 14 | 11 | 17 | 13 |
| Healthcare will be an important issue to me, but less important than other issues | 54 | 55 | 64 | 57 |
| Healthcare will not be a very important issue to me in the election | 19 | 29 | 12 | 24 |
| I do not plan to vote on November 7th | 13 | 5 | 7 | 7 |
Let's try to make that 13% of folks not voting a bit smaller...
May your favorite candidate win!
-Wes
Sunday, November 05, 2006
Finding Big Veins Safely
I'm in yet another city preparing for another talk to doctors who (reportedly) are interested in my experiences (can you believe?). It's a chance to share experiences - hopefully so others can avoid the difficulties I have encountered during my learning curve doing complicated (and not-so-complicated) pacemaker implantation. Typically, these talks are well-received - in part because you get to show tough cases and the audience can smile politely as if to say, "Better you than me!"
Anyway, I was preparing for this talk and wondered if some of the information might be helpful of interesting to the blog-o-sphere. In addition, if it helps avoid a complication for a patient, then my blog will be worth the work.
I use this technique to find a big vein (called the "axillary vein") in the upper chest area (just beneath the collar bone or "clavicle") where we implant pacemaker and defibrillator leads. I have been impressed at how few doctors use a bit of help for this access. (Some might call this access a "subclavian venous access," but because the access is made lateral to the clavicle, and not beneath it, it is called an "axillary venous" access approach.)
My technique? I cheat.
You see I have come to learn that the anatomic course the axillary and subclavian veins traverse can be quite variable from patient to patient, especially the elderly. And in whom do we place the most pacemakers? The elderly. A colleague of mine exposed me to a new tool to definitively identify the vein: ultrasound. Using sound waves to find the veins can be extremely helpful and expedites access to the veins. Here's what our (older model) machine looks like:
There are two probes that use different frequencies of sound to provide the image at 5.0 and 7.5 MHz. The 7.5 MHz probe has better resolution but poorer penetration in thick tissues (better for internal jugular access). I tend to use the 5.0 MHz probe most often:

Once the probe is chosen, we place some ultrasound gel into a plastic bag, and then place the selected probe into the plastic bag (ultrasound doess not travel well through air). This gel facilitates imaging of the vein:

The probe is then placed into the sterile gel-filled plastic bag, and the bag secured onto the probe with little rubber bands:
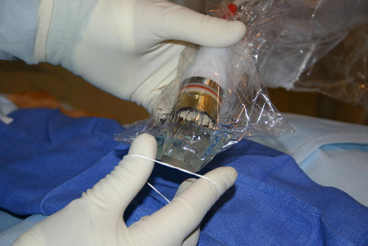
A small amount of sterile gel is applied to the surface of the skin as well, then imaging of the vein and artery performed by moving the probe around beneath the calvicle until two dark echo-lucent vessels are indentified. With the ridged edge of the probe toward the operator, the vein is imaged in the same anatomic relationship as the actual anatomy (A = Artery, V = Vein):

Applying gentle pressure on the skin over the vein compresses the vein but not the artery as seen:
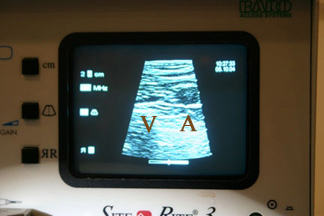
After identifying the vein, imaging during puncture of the vein can be accomplished safely.
I have found this technique has helped improve the safely and efficacy of performing axillary or subclavian vein access (for pacemaker placement or central lines). If you don't have such a machine, you might want to think of getting one. You can learn more about this instrument here. (Note: I have no relationship with the company - just hope this might help someone else like it has helped me and my patients).
-Wes
Anyway, I was preparing for this talk and wondered if some of the information might be helpful of interesting to the blog-o-sphere. In addition, if it helps avoid a complication for a patient, then my blog will be worth the work.
I use this technique to find a big vein (called the "axillary vein") in the upper chest area (just beneath the collar bone or "clavicle") where we implant pacemaker and defibrillator leads. I have been impressed at how few doctors use a bit of help for this access. (Some might call this access a "subclavian venous access," but because the access is made lateral to the clavicle, and not beneath it, it is called an "axillary venous" access approach.)
My technique? I cheat.
You see I have come to learn that the anatomic course the axillary and subclavian veins traverse can be quite variable from patient to patient, especially the elderly. And in whom do we place the most pacemakers? The elderly. A colleague of mine exposed me to a new tool to definitively identify the vein: ultrasound. Using sound waves to find the veins can be extremely helpful and expedites access to the veins. Here's what our (older model) machine looks like:

There are two probes that use different frequencies of sound to provide the image at 5.0 and 7.5 MHz. The 7.5 MHz probe has better resolution but poorer penetration in thick tissues (better for internal jugular access). I tend to use the 5.0 MHz probe most often:

Once the probe is chosen, we place some ultrasound gel into a plastic bag, and then place the selected probe into the plastic bag (ultrasound doess not travel well through air). This gel facilitates imaging of the vein:

The probe is then placed into the sterile gel-filled plastic bag, and the bag secured onto the probe with little rubber bands:

A small amount of sterile gel is applied to the surface of the skin as well, then imaging of the vein and artery performed by moving the probe around beneath the calvicle until two dark echo-lucent vessels are indentified. With the ridged edge of the probe toward the operator, the vein is imaged in the same anatomic relationship as the actual anatomy (A = Artery, V = Vein):

Applying gentle pressure on the skin over the vein compresses the vein but not the artery as seen:

After identifying the vein, imaging during puncture of the vein can be accomplished safely.
I have found this technique has helped improve the safely and efficacy of performing axillary or subclavian vein access (for pacemaker placement or central lines). If you don't have such a machine, you might want to think of getting one. You can learn more about this instrument here. (Note: I have no relationship with the company - just hope this might help someone else like it has helped me and my patients).
-Wes
Medicare to Cut Physician Payments by 5%
Just in time for the elections, the big news from the conference I attended this weekend was that a 5% paycut for physician services from Medicare will take place effective 1 Jan 2007. From CMS:
-Wes
The Medicare law includes a statutory formula that will require CMS to implement a minus 5.0 percent update in payment rates for physician-related services. This is slightly less than the 5.1 percent reduction in the proposed rule. This formula compares the actual rate of growth in spending to a target rate, which is based on such factors as the growth in number of Medicare fee-for-service beneficiaries and statutory or regulatory changes in benefits. If the actual rate of spending growth exceeds the target rate, the update is decreased; if it is less, the update is increased. Every year beginning with 2002, in response to rising spending, the statutory update formula would have operated to impose payment cuts. The negative update went into effect in 2002, but for 2003 to 2006, Congress intervened and temporarily suspended the requirements of the formula in favor of specific, statutory updates.No such action occured by Congress this year (as expected), so as of 1 Jan 2007 doctors will need to start making some business decisions. CMS's press release was sugar-coated, stating:
“The rule we are announcing today will pay physicians more for the time they spend talking with their patients about their health care,” said Leslie V. Norwalk, CMS Acting Administrator. “We believe that this emphasis on personalized care will lead to better outcomes for patients, and more efficient use of health care resources.”The Final Rule will take some time to evaluate its effect on individual physician subspecialties, but I feel cardiovascular and orthopedic services will likely be hit the hardest.
-Wes
Saturday, November 04, 2006
Movin' On

Well here's my last (poor) photo of my current location. It's another clue, you see it's the side view of a local convention center. Note also it's SUNNY, and WARM here. But I must go. On to my next road warrior location (stay tuned). Oh, the ducks seen of the prior photo? They're on a roof-top of my hotel here. Check the comments for the where this is if you give up...
-Wes
Friday, November 03, 2006
Lunchtime Medical Education
I think it's interesting that some medical schools are helping our medical students learn how to deal with the pharmaceutical sales rep pitches at lunchtime by "appealing to physicians' natural skepticism." But my skepticism meter registers more about the effectiveness of this teaching. I have been more impressed that there is usually little pitch offered by reps when they bring lunch: they seem just as happpy to take a break for lunch as those they're feeding. So any medical student or resident who lashes into a sales rep "nice" enough to bring in lunch would likely be perceived as impolite or cocky, wouldn't they? So will doctors really challenge the reps if they are perceived by their peers this way?
Even worse is when you're successful at poking a hole in one of the drug rep's claims (which is quite easy). Then the rep has an excuse to return to your office again with a "clarification" or literature search.
And then they're back again, aren't they. In your face.
-Wes
Even worse is when you're successful at poking a hole in one of the drug rep's claims (which is quite easy). Then the rep has an excuse to return to your office again with a "clarification" or literature search.
And then they're back again, aren't they. In your face.
-Wes
Globo-health
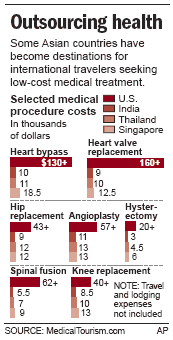 With testimonials, press coverage, and costs like these, the new global era of health care has arrived.
With testimonials, press coverage, and costs like these, the new global era of health care has arrived.Dodie Gilmore is a spry 60-year-old who loves the outdoors, but when she could no longer straddle her faithful horse, River, she knew it was time for a new hip.And Coldwell Banker is not the only one thinking about this arrangement:
But how could she afford it? As an independent contractor for a small Coldwell Banker real estate franchise in Durant, Okla., she knew her privately purchased health plan would never pay up to $40,000 for the operation.
So she asked her boss about traveling to India where hip resurfacing alone would cost just $7,000. He not only gave her his blessing but offered to foot the bill, minus travel and hotels — making Gilmore one of the very first Americans sent overseas for surgery by an employer.
United Group Programs, a Boca Raton, Fla.-based company that sells self-insurance policies to small businesses, is already offering a plan that sends patients to Bumrungrad International hospital in Bangkok, Thailand. UGP says the plan will save employers more than 50 percent on major medical costs and slash employees’ out-of-pocket expenses to zero.Non-union employees seem particularly vulnerable (or fortunate, depending on which side of the debate you favor). But when United Steelworkers union blocked a North Carolina employee of Blue Ridge Paper Products in Canton, N.C. from receiving a gall bladder resection in India, they exposed an contentious issue:
Blue Shield of California and Health Net of California also both offer lower-cost policies allowing members to seek medical care in Mexico.
In June, David Boucher, an assistant vice president at BlueCross BlueShield of South Carolina, traveled to Bangkok for a close-up look at Bumrungrad. The Thai hospital began heavily recruiting overseas patients after the 1997 Asian financial crisis. It drew 400,000 foreigners last year — including 55,000 Americans.
“I was thoroughly impressed,” Boucher said. “We’re taking a serious look at this as an alternative” for the health plan’s 1.5 million members.
The union’s resistance has brought to the fore a critical question in the path of the globalization of the health care industry — who is liable if something goes wrong in an overseas hospital? And underlying all this is the even more explosive issue of potential job losses in the American health care industry, in an economy already sensitive to the large-scale shift of jobs to cheaper overseas locations.I have a feeling I know who will win this battle. It's a dog-eat-dog world out there, isn't it?
Now for the controversy: should we be training our physician competitors?
-Wes
Thursday, November 02, 2006
Police Captain Sues Everyone After Heart Attack
Oh, geez, just when I'm trying to get on a plane I read this:
And we wonder why health care costs are skyrocketing...
-Wes
PS: The captain should consider reading this book. It will put his health problems in perspective.
The suit, filed by attorney Michael Lucas, is seeking compensation for physical and mental pain suffered by former police captain Gordon Carter, who left the police department after he had a heart attack in July 2005.To think the poor El Capitan was "forced" to go through rehab... what were those doctors thinking?
According to the suit, Dr. Thomas Donahue implanted a Medtronic ICD pacemaker, or internal cardiac defibrillator, to correct Carter's heart problem in August 2005. After testing two months later, the pacemaker was found to be defective and it was replaced with another Medtronic device.
Now Carter is suing Medtronic, Inc., the city of Pikeville, the Pikeville Police Department, the Kentucky League of cities, its insurance service agency and workers' compensation fund as well as unknown defendants associated with the manufacturing and distribution of the Medtronic pacemaker.
Lucas claims that Carter was injured by the “unreasonably unsafe hazardous product” because it was defective. Carter was “forced” to go through cardiac rehabilitation, delayed recovery, depression, pain, “attendant worries” and additional medical expenses because of the defective pacemaker, he wrote in the suit.
He alleges that the company, by manufacturing and distributing the device, implied that it was safe, and he argues that they caused harm to Carter by failing to warn him or his doctor about the potential dangers.
Lucas claims that city officials accepted Carter's heart attack as a work-related injury, but city officials say they don't have the authority to make that determination.
And we wonder why health care costs are skyrocketing...
-Wes
PS: The captain should consider reading this book. It will put his health problems in perspective.
Ramblin' Man
I'll be on the road for a few days "tryin' to make a livin' and doin' the best I can" (as the song goes). Blogging might suffer a but, but, heck it'll be good to take a little break...might freshen the sole a bit...
I've noticed my rant-o-meter's a bit low...
-Wes
I've noticed my rant-o-meter's a bit low...
-Wes
Wednesday, November 01, 2006
Heart Failure: Why Wait Until Extremes?

Today's New England Journal of Medicine disclosed the effectiveness of a left ventricular assist device (LVAD) and medical regimen at reverse-remodeling chronically dilated hearts back to near-normal in a small subset of 15 patients. While these data were novel and encouraging - one wonders if these individuals could have been spared the need for left-ventricular assist devices if they had had implementation of biventricular pacing earlier in their clinical course.
I was unable to find mention of the EKG duration of the patients followed in the New England Journal of Medicine article, nor did it appear that ANY of these patients had received a biventricular pacing device. I suppose I should not be surprised, since the New England Journal of Medicine study was funded by the LVAD manufacturer, Thoratec. But excluding this data omits important data regarding these severe heart failure patients: was all done for these patients before LVAD implantation? Although I appreciate that not all heart failure can be detected early, 12 of 15 of the patients in this study had been treated for at least 6 months before LVAD implantation without biventricular pacing, leading me to wonder if the implantation of a biventricular device could have prevented the need for the LVAD.
Biventricular pacing has now been firmly established as an effective means of treating patients with severe congestive heart failure on maximal medical therapy. It should probably be considered the standard of care, in my view, for patients with severe cardiomyopathy refractory to medical therapy with evidence of conduction delay during activation of the left ventricle (QRS duration >=120 msec). Biventricular pacing involves placing a left ventricular pacing lead in addition to a right ventricular pacing lead to re-coordinate the pumping action of the ventricular pumping chambers. Clinical studies have demonstrated that approximately 2/3rds of symptomatic patients have an improvement in their 6-minute hall walk test (walking on average an additional 50 meters), improve by about one New Heart Association heart failure class, and have improved quality of life using self-assessment measures. More importantly, the COMPANION and recently-released CARE-HF trials have demonstrated a mortality benefit to patients receiving biventricular pacing devices. Anecdotally, I have seen complete normalization of left ventricular function in a small subset of patients with non-ischemic cardiomyopathy (like those the the NEJM article) after this therapy has been deployed.
It should be noted that the effect of biventricular pacing trials has been so impressive that earlier intervention of biventricular pacing in heart failure is now being evaluated in the BLOCK-HF trial and its application to patients with normal EKG duration in St. Jude Medical's RethinQ trial.
Hopefully we'll remember the benefit of biventricular pacing therapy (with or without an implantable defibrillator) in our sickest heart failure patients and apply this before the need for an LVAD arises.
-Wes
Photo credit.
Torcetrapib and Hypertension - Glass Half Empty?
It is interesting that Pfizer’s drug torcetrapib – a cholesterol lowering drug developed to raise HDL (or “good cholesterol”) – was found to raise systolic blood pressure by 2-4 millimeters of mercury. Wall Street and its analysts seem concerned. While it is useful in large trials to monitor important trends like this due to known risk factors of hypertension such as stroke, could this side effect be beneficial?
Many patients I see with severe New York Heart Association Class III or Class IV heart failure often have very low blood pressure, since their systolic function (or ability of the heart muscle to generate pressure) is compromised. It is well known that elevated blood pressure increases the myocardial work (and hence oxygen requirements). However, many of our treatments known to improve survival in patients with heart failure lower blood pressure significantly (like ACE inhibitors and beta blockers) to such an extent, their dosage has to be limited. Many a clinician would welcome a drug that might permit higher amounts of these known beneficial drugs to be used on their patients, provided there were no other adverse side effects in doing so.
I hope the FDA does not act too quickly here and disapprove this drug before more information regarding torcetrapib become available. There might be a benefit to seeing the glass half full instead of half empty.
-Wes
Many patients I see with severe New York Heart Association Class III or Class IV heart failure often have very low blood pressure, since their systolic function (or ability of the heart muscle to generate pressure) is compromised. It is well known that elevated blood pressure increases the myocardial work (and hence oxygen requirements). However, many of our treatments known to improve survival in patients with heart failure lower blood pressure significantly (like ACE inhibitors and beta blockers) to such an extent, their dosage has to be limited. Many a clinician would welcome a drug that might permit higher amounts of these known beneficial drugs to be used on their patients, provided there were no other adverse side effects in doing so.
I hope the FDA does not act too quickly here and disapprove this drug before more information regarding torcetrapib become available. There might be a benefit to seeing the glass half full instead of half empty.
-Wes
Subscribe to:
Comments (Atom)

