 |
| Sgt Bernie Goulet, Spring, 1951 Korea |
He sat before me, remembering.
"I was 19 back then. Too long ago. You know, there were some things you never forget. One of them was my company commander, Capt Harold Willecke. Great guy. Somehow he took me under his wing - my mentor. Showed me the ropes, how to fight. We were pretty effective, had plenty of successful engagements against the enemy."
As the surrounding conversation became muted by his hearing aides, his eyes, twinkling and animated, were fixed on me as he continued.
"There was one time with Willecke I'll never forget. We were pinned down, the Chinese advancing all around us. Staying put was certain slaughter. Willecke knew we had to move, but most of us were too scared. Willecke wouldn't have any of it! He got up and started running, gun blazing. I followed right behind. His actions got the whole group of us going. But he never saw the hidden bunker to his right. I saw a three or four shots from a burp gun rip across his chest. The thing about a burp gun is it's not as powerful as a machine gun. If it had been a machine gun, the rounds probably would have gone through him and hit me. He fell forward face-first right in front of me. I heard just a slight groan, then a few kicks of his legs, then nothing."
"There was one time with Willecke I'll never forget. We were pinned down, the Chinese advancing all around us. Staying put was certain slaughter. Willecke knew we had to move, but most of us were too scared. Willecke wouldn't have any of it! He got up and started running, gun blazing. I followed right behind. His actions got the whole group of us going. But he never saw the hidden bunker to his right. I saw a three or four shots from a burp gun rip across his chest. The thing about a burp gun is it's not as powerful as a machine gun. If it had been a machine gun, the rounds probably would have gone through him and hit me. He fell forward face-first right in front of me. I heard just a slight groan, then a few kicks of his legs, then nothing."
He paused again to regain his composure. After a moment, ignoring all of the other conversations underway around the Memorial Day picnic table, be continued.
"Hey, you know what my son did?"
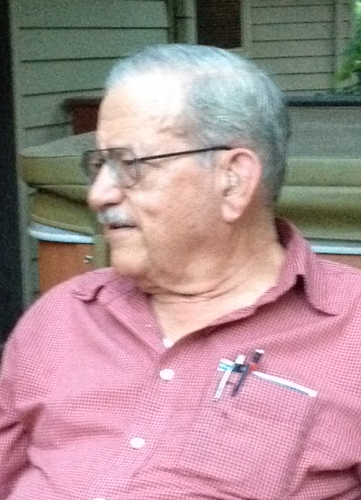 |
| Bernie Goulet, Memorial Day 2012 |
Then suddenly, the present day returned as his daughter's voice broke through:
"Hey Bernie, try some of this cheese I brought or maybe a little of this wine?"
-Wes
PS: Bernie's photo collection, courtesy of the Lincoln Library.








